MIT researchers have developed a breakthrough mRNA vaccine adjuvant that reprograms dendritic cells to generate significantly more powerful T-cell responses, capable of eradicating tumors in mouse models and potentially revolutionizing cancer treatment and infectious disease prevention.
Researchers at MIT and Massachusetts General Hospital have unveiled a novel approach to cancer vaccination that leverages immune-remodeling mRNA molecules to generate T cells with unprecedented tumor-fighting capabilities. This technology has demonstrated remarkable success in preclinical models, with the ability to slow tumor growth and, in many cases, completely eradicate various forms of cancer.
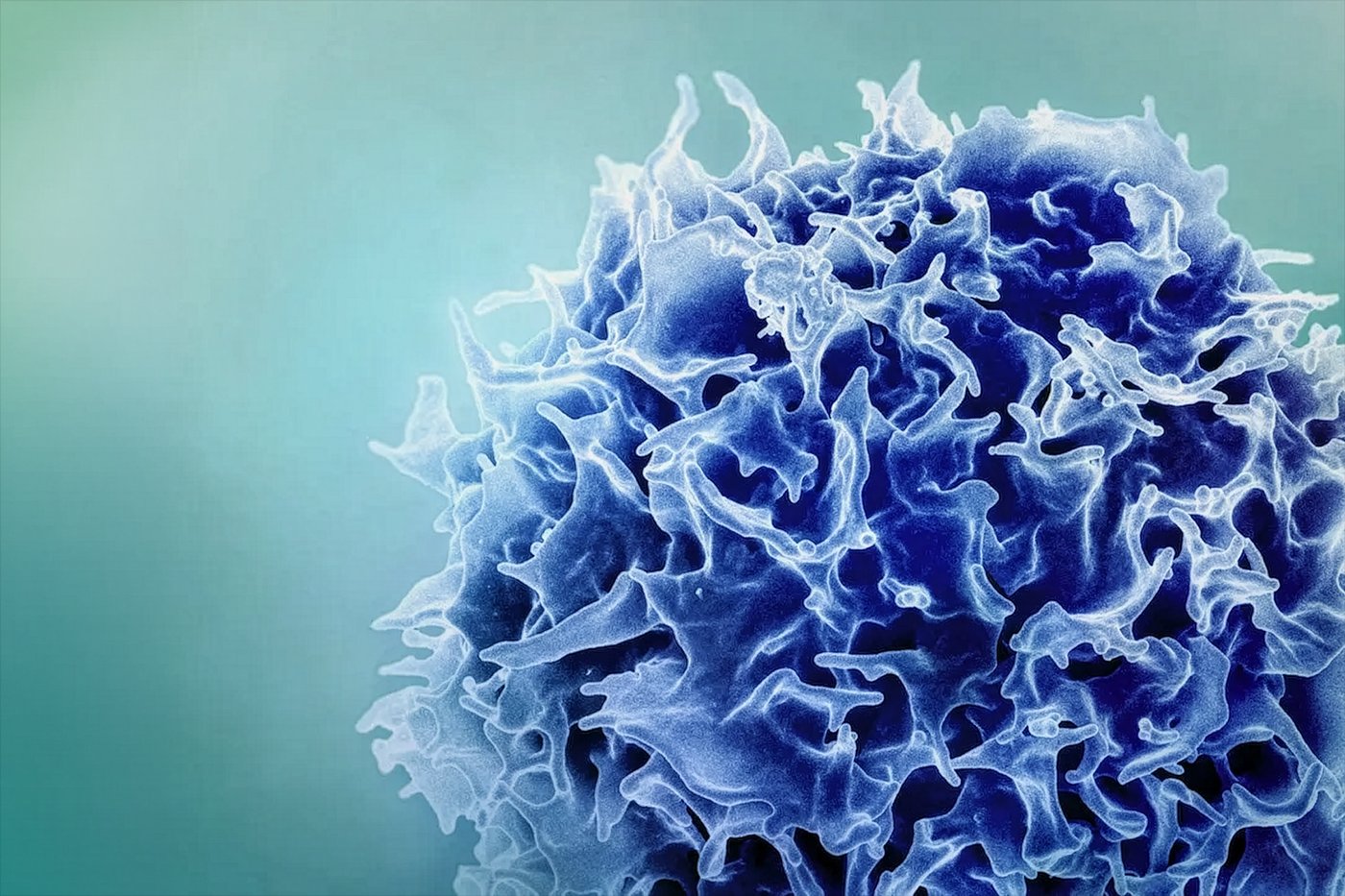
The core innovation lies in a new type of vaccine adjuvant—a substance that enhances the body's immune response to a vaccine. Unlike traditional adjuvants, this approach utilizes mRNA strands encoding two specific genes: IRF8 and NIK. These genes play critical roles in antigen presentation and can switch immune cells into a more active state, effectively creating a "supercharged" T-cell response.
"Most vaccines generate both antibodies and T cells that can target the vaccine antigen by activating antigen-presenting cells, such as dendritic cells," explains Daniel Anderson, a professor in MIT's Department of Chemical Engineering and a member of MIT's Koch Institute for Integrative Cancer Research. "In this study, we boosted the T-cell response with a new type of vaccine adjuvant that consists of mRNA molecules encoding genes that turn on immune signaling pathways and promote a much more powerful T-cell response."
The technical approach involves packaging these mRNA molecules in specially designed lipid nanoparticles that, after intravenous injection, target the spleen—a key hub for immune cell activity. Unlike the lipid nanoparticles used in COVID-19 vaccines, these have a different chemical composition optimized for spleen delivery.
Within the spleen, these particles encounter antigen-presenting cells, including dendritic cells. Once inside these cells, the mRNA is translated into proteins, including the IRF8 transcription factor and the NIK enzyme. NIK activates a signaling pathway crucial for immunity and inflammation, while IRF8 helps program dendritic cells, particularly a subset called cDC1, which are exceptionally effective at activating T cells.
"We see that the dendritic cells start shifting toward a more cDC1 phenotype, which is the most important dendritic cell phenotype and can generate a stronger T-cell response," says Akash Gupta, lead author of the study and now an assistant professor at the University of Houston.
This immune remodeling occurs rapidly—within 24 hours of administration. The activated dendritic cells then prime an anti-tumor response, leading to an expansion of T-cell populations over several days to a week. These enhanced T cells, working alongside other immune cells such as natural killer (NK) cells, can recognize and attack tumors with remarkable efficiency.
The researchers tested this approach across multiple mouse models of aggressive cancers, including bladder cancer, colon carcinoma, melanoma, and metastatic lung cancer. In nearly all cases, the injected mRNA stimulated a robust T-cell response that significantly slowed tumor growth and frequently led to complete tumor eradication.
"Most cancer immunotherapies rely on external signals to activate immune cells. We take a different approach—reprogramming immune cells from within by targeting their internal signaling machinery, enabling a more potent and durable anti-tumor response," says Riddha Das, another lead author.
What makes this approach particularly promising is its versatility. The mRNA adjuvant worked effectively even when administered without a specific cancer antigen, simply by broadly activating the immune system. However, combining it with cancer-specific antigens created an even more powerful response.
The technology also demonstrated synergy with existing immunotherapies. When combined with checkpoint blockade inhibitors—drugs that work by lifting a brake that tumor cells place on T cells—the adjuvant significantly enhanced their effectiveness. This is particularly important because checkpoint inhibitors alone don't work for all patients.
"The microenvironment of solid tumors is often hostile to T cells and represents a major barrier to effective immunotherapy. We find that immune remodeling with these adjuvants creates a T cell–permissive environment and promotes tumor rejection," notes Christopher Garris, assistant professor at Harvard Medical School and Massachusetts General Hospital.
Beyond cancer applications, the researchers explored whether this adjuvant could enhance protection against infectious diseases. When delivered alongside COVID-19 or influenza vaccines, the mRNA adjuvant generated a 10-to-15-fold stronger T cell response in mice compared to the vaccines alone.
"While there are differences between the mouse systems that we've worked in and humans, we are optimistic that these adjuvants will work in humans and could improve a range of different vaccines," Anderson says.
The potential advantages of this approach over previous immunostimulatory strategies are significant. Direct administration of cytokines—immune-stimulating molecules—has been attempted but often leads to overstimulation of the immune system and potentially severe side effects. The mRNA-based approach offers a more targeted and controlled method of immune activation.
The technology builds upon the success of mRNA vaccines developed during the COVID-19 pandemic but represents a significant advancement. Where COVID vaccines primarily focused on generating antibodies against the spike protein, this new approach specifically enhances the cellular arm of the immune system—the T cells that are crucial for fighting cancer and clearing viral infections.
Looking ahead, the researchers plan to test this approach in additional animal models with the goal of developing it for clinical use in both cancer and infectious diseases. The research was funded by Sanofi, the National Institutes of Health, the Marble Center for Cancer Nanomedicine, and the Koch Institute Support (core) Grant from the National Cancer Institute.
The full study, titled "Immune-remodeling mRNAs expressing IRF8 or NIK generate durable antitumor immunity in multiple cancer models," was published today in Nature Biotechnology and represents a significant step forward in the field of cancer immunotherapy and vaccine development.
For more information on this research, you can explore the original article in Nature Biotechnology or visit the Anderson Lab at MIT for additional details on their work in mRNA delivery and immunotherapy.
Comments
Please log in or register to join the discussion