MIT engineers have developed injectable mini livers that could provide an alternative to transplantation for thousands of patients with liver failure.
More than 10,000 Americans with chronic liver disease are waiting for a liver transplant, but donor organs remain scarce. Now, MIT engineers have developed a groundbreaking approach that could help these patients without requiring major surgery: injectable "mini livers" that take over the functions of a failing liver.
These engineered tissue grafts, described in a new study published today in Cell Biomaterials, could serve as "satellite livers" that provide critical liver functions while leaving the diseased organ in place. The research, led by Sangeeta Bhatia, the John and Dorothy Wilson Professor of Health Sciences and Technology and of Electrical Engineering and Computer Science at MIT, represents a potential paradigm shift in treating liver disease.
How the Technology Works
The key innovation involves injecting hepatocytes—the liver cells responsible for most of the organ's functions—along with specially designed hydrogel microspheres. These microspheres create an engineered niche that helps the cells survive and integrate with the body's circulatory system.
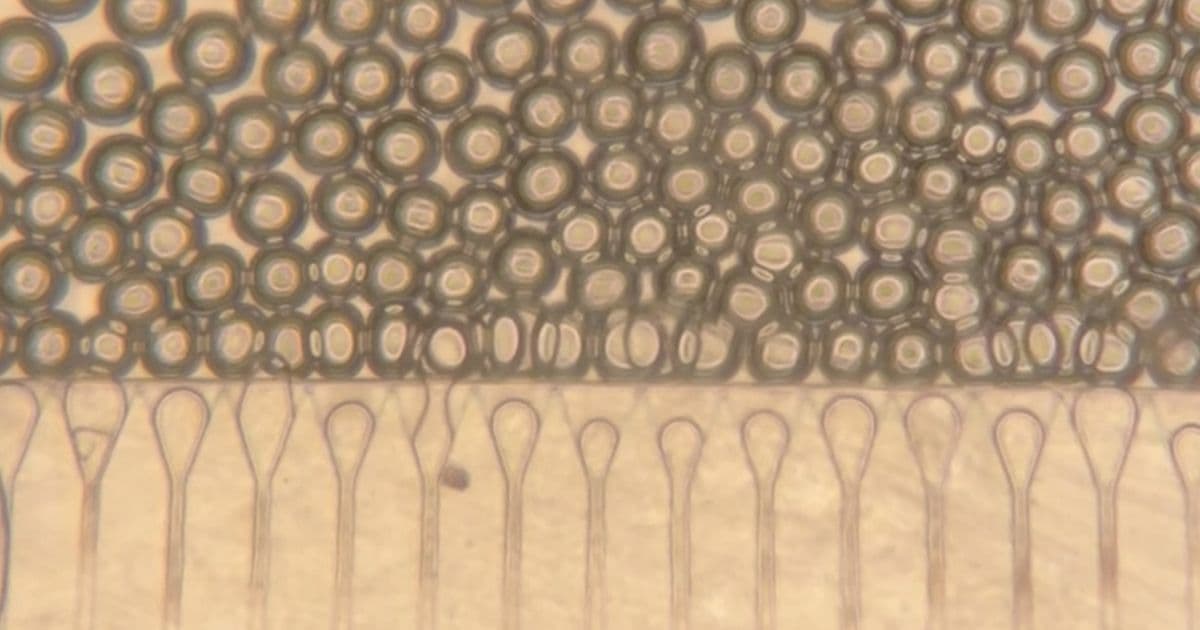
Researchers used a microfluidic device to generate hydrogel microspheres of uniform shape and size. These spheres are then mixed with hepatocytes and injected into the body, where they form stable mini livers. Credit: Courtesy of the Bhatia Lab
The microspheres have unique properties that allow them to behave like a liquid when packed together, making them injectable through a syringe. Once inside the body, they regain their solid structure and create spaces where hepatocytes can migrate, build connections, and form functional tissue.
"What we did is use this technology to create an engineered niche for cell transplantation," explains Vardhman Kumar, the paper's lead author and MIT postdoc. "If the cells are injected in the absence of these spheres, they would not integrate efficiently with the host, but these microspheres provide the hepatocytes with a niche where they can stay localized and become connected to the host circulation much faster."
Promising Results in Animal Studies
In tests with mice, the researchers injected the cell-microsphere mixture into fatty tissue in the belly. Over time, the injected cells formed stable, compact structures. Blood vessels grew into the graft area, providing nutrients and enabling the hepatocytes to function normally.
"The new blood vessels formed right next to the hepatocytes, which is why they were able to survive," Kumar says. "They were able to get the nutrients delivered right to them, they were able to function the way they're supposed to, and they produced the proteins that we expect them to."
The injected hepatocytes remained viable and continued secreting specialized proteins into the host circulation for eight weeks—the length of the study. This suggests the therapy could potentially work as a long-term treatment for liver disease.
A Bridge to Better Treatment
The researchers envision several applications for this technology. It could serve as an alternative to surgery for patients who aren't healthy enough for a transplant, or as a "bridge" therapy that supports patients while they wait for a donor organ to become available.
"The way we see this technology is it can provide an alternative to surgery, but it can also serve as a bridge to transplantation where these grafts can provide support until a donor organ becomes available," Kumar explains. "And if we think they might need another therapy or more grafts, the barriers to do that are much less with this injectable technology than undergoing another surgery."
Technical Advantages
One of the most significant advantages of this approach is its versatility. Unlike traditional tissue engineering approaches that require surgical implantation of large hydrogel constructs, these injectable mini livers can be delivered through a simple injection guided by ultrasound.
Working with Nicole Henning, an ultrasound research specialist at the Koch Institute, the researchers developed a way to inject the cell mixture using a syringe guided by ultrasound. After injection, the researchers can also use ultrasound to monitor the long-term stability of the implant.
This means the therapy could potentially be delivered to various sites in the body—not just near the liver. As long as there's enough space and access to blood vessels, the injected hepatocytes can function similarly to those in a natural liver. "For a vast majority of liver disorders, the graft does not need to sit close to the liver," Kumar notes.
Future Directions
While the current version of this technology would likely require patients to take immunosuppressive drugs, the researchers are exploring ways to make the hepatocytes "stealthy" enough to evade the immune system. They're also investigating using the hydrogel microspheres to deliver immunosuppressants locally, which could reduce side effects.
The research was funded by multiple sources including the National Institutes of Health, the National Science Foundation, and the Howard Hughes Medical Institute. The team's work builds on over a decade of research in Bhatia's lab aimed at restoring hepatocyte function without requiring a full liver transplant.
For the thousands of patients currently waiting for liver transplants—and the many more who aren't eligible for surgery—these injectable mini livers could represent a transformative new option. By providing critical liver functions through a simple injection rather than major surgery, this technology could dramatically expand treatment possibilities for liver disease.
The microspheres (green), hepatocytes (magenta), and supporting fibroblasts (orange) assemble and reorganize into engineered liver grafts over time. Image shows a comparison of day zero (left) and day fourteen (right) of the grafts cultured in the laboratory. Credit: Courtesy of the Bhatia Lab
As Kumar puts it, these are "satellite livers"—additional functional liver tissue that could provide crucial support without replacing the entire organ. For patients with few treatment options, that could make all the difference.
Comments
Please log in or register to join the discussion