UC Davis Health researchers have successfully performed the world's first in-utero stem cell therapy for spina bifida, combining fetal surgery with placental-derived stem cells in a landmark clinical trial.
A UC Davis Health research team has achieved a medical milestone by safely performing the world's first spina bifida treatment that combines fetal surgery with stem cells, according to results from Phase 1 of an ongoing clinical trial published today in The Lancet. The study, called "Feasibility and Safety of Cellular Therapy for In-Utero Repair of Myelomeningocele (CuRe Trial)," tested whether adding a layer of human placenta-derived stem cells to standard fetal surgery could be done safely.
Spina bifida, also known as myelomeningocele, occurs when spinal tissue fails to fuse properly during the early stages of pregnancy. This birth defect can lead to a range of lifelong cognitive, mobility, urinary and bowel disabilities, affecting 1,500 to 2,000 children in the United States every year.
[IMAGE:1]
"Putting stem cells into a growing fetus was a total unknown. We are excited to report great safety," said Diana Farmer, the CuRe Trial's principal investigator and chair of the UC Davis Department of Surgery. "It paves the way for new treatment options for children with birth defects. The future is exciting for cell and gene therapy before birth."
How the Treatment Works
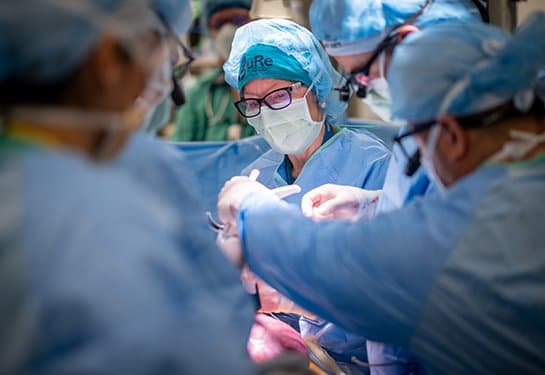
During fetal surgery, surgeons make a small opening in the uterus and carefully position the fetus to access the spina bifida defect. The care team then places a small patch containing living stem cells directly over the fetus's exposed spinal cord before closing the layers of the back to allow tissue regeneration.
The stem cells, taken from donated placentas, are designed to protect the developing spinal cord from further damage before birth. This represents the world's first in-utero stem cell therapy for spina bifida and the only trial aimed at improving outcomes beyond fetal surgery alone.
Key Safety Findings
The first six babies in the trial were monitored closely from surgery through birth. Researchers reported:
- No safety concerns related to the stem cells
- No infections, spinal fluid leaks, or abnormal tissue growth
- No tumors formed at the repair site
- All surgeries were successful with the stem cell patch placed as planned
- All wounds were completely healed
- MRI scans showed reversal of hindbrain herniation in all infants, an indicator of surgical success
- No babies required a shunt for hydrocephalus before hospital discharge
Because the early safety results were strong, the Food and Drug Administration and an independent monitoring board approved moving forward with the next phase of the study.
Why This Matters
While fetal surgery has greatly improved outcomes since its introduction more than a decade ago, many children with spina bifida still struggle with mobility and have other long-term complications. The CuRe Trial is exploring whether stem cells can add regenerative power to surgery, potentially improving mobility and quality of life.
"This is a major step toward a new kind of fetal therapy, one that doesn't just repair but potentially helps heal and protect the developing spinal cord," said Aijun Wang, co-inventor of the placental-derived stem cell treatment technology and the study's co-principal investigator with Farmer. He is co-director of the UC Davis Center for Surgical Bioengineering.
For CuRe Trial participant Michelle Johnson, the decision to participate in the trial was life changing. "Our family couldn't feel more blessed and fortunate to participate in the CuRe Trial," said Johnson, whose son Tobi was born in 2022. "Tobi's physical and mental abilities are nothing short of a miracle. We are forever grateful for the many health professionals who supported Tobi's journey and continue to watch him conquer the world."
[IMAGE:2]
Next Steps
The CuRe trial is now enrolling up to 35 patients in its Phase 1/2a study. Children will be followed through age 6 to evaluate long-term safety and early signs of improved movement, bladder and bowel function. The Phase 1/2a study is funded by CIRM and Shriners Children's.
The first phase of the trial was funded by a $9 million state grant from the California Institute for Regenerative Medicine (CIRM), highlighting the significant investment in this groundbreaking research.
Comments
Please log in or register to join the discussion